Contents
Impetigo
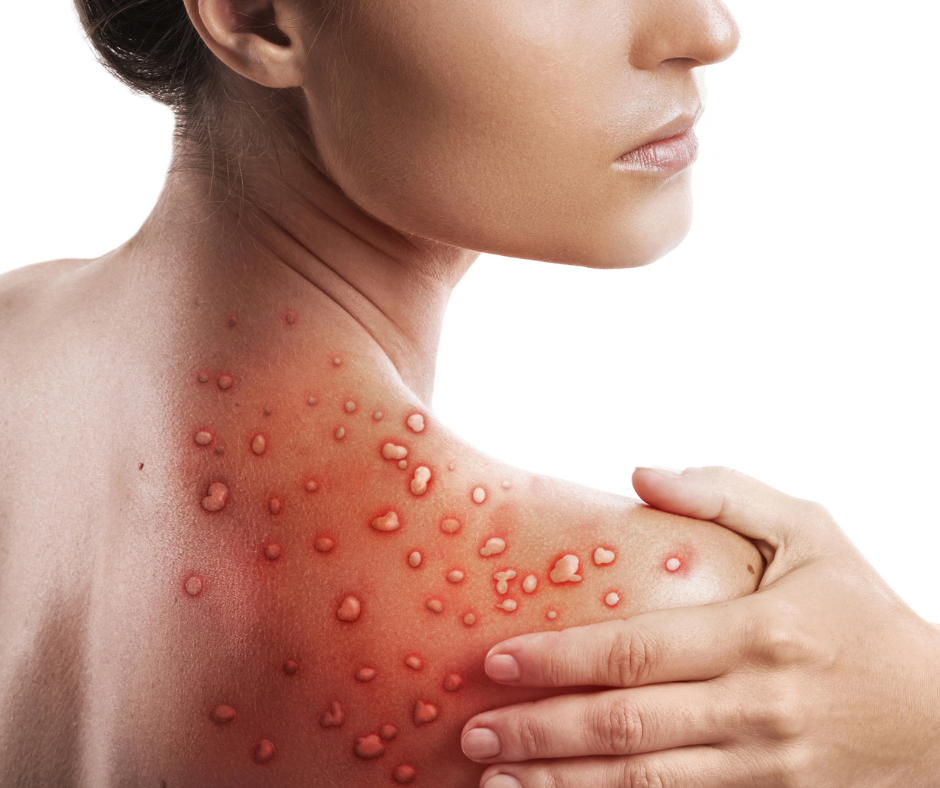
Impetigo is a highly prevalent bacterial skin infection characterized by superficial, scattered pustules that rapidly rupture and form honey-colored crusts. It’s particularly common in young children, though adults can also be affected. If left untreated, impetigo can lead to both localized and systemic complications.
Etiology:
- Causative Agents: Staphylococcus aureus, Streptococcus species, or a combination of both.
- Predisposing Factors: Young age, hot and humid climates, poor hygiene, and underlying skin conditions such as scabies, lice infestations, insect bites, and atopic dermatitis.
Furuncles
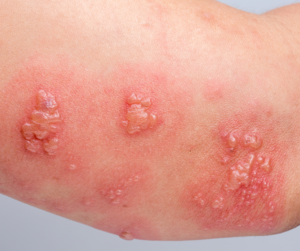
A furuncle, commonly known as a boil, is an acute inflammatory condition characterized by necrosis of the hair follicle and surrounding tissue. This type of skin infection is frequently observed during the summer months and tends to affect males more often than females. While it can occur at any age, it is more prevalent in children.
Etiology
The primary causative agent of furuncles is Staphylococcus aureus. This bacterium is a normal inhabitant of the skin, particularly colonizing hair follicles in areas such as the nasolabial folds, intergluteal cleft, and the nasal vestibule. When a hair follicle sustains damage, coupled with predisposing factors like weakened immunity, malnutrition, or diabetes, S. aureus can proliferate and initiate infection.
Folliculitis
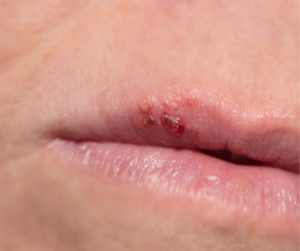
Folliculitis is a common skin condition characterized by inflammation of one or more hair follicles. It can occur at any age, but is particularly prevalent in adolescents and young adults.
Etiology
- Bacterial: The most common culprits are Staphylococcus aureus and Pseudomonas aeruginosa.
- Fungal: Trichophyton rubrum and Malassezia folliculitis (formerly Pityrosporum folliculitis) are frequently implicated.
- Viral: Herpes simplex virus can cause folliculitis, especially around the mouth.
- Non-infectious:
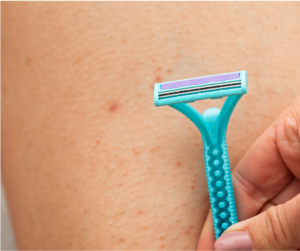
- Pseudofolliculitis barbae: Often seen in the beard area due to shaving, resulting in ingrown hairs.
- Eosinophilic folliculitis: Commonly affects individuals with compromised immune systems.
- Folliculitis decalvans: Primarily affects the scalp, leading to permanent hair loss.
- Occupational folliculitis: Occurs in individuals exposed to oils and greases, such as oil refinery workers and mechanics.
Predisposing Factors
Local
- Occlusive clothing
- Skin maceration
- Hyperhidrosis
- Scratching or excoriation
- Shaving
- Plucking hairs
- Irritating medications or cosmetics
- Prolonged topical corticosteroid use
Systemic
- Obesity
- Diabetes mellitus
- Immunosuppression (congenital or acquired)
- Renal failure, hemodialysis
- Iron deficiency anemia (sometimes associated with chronic cases)
Staphylococcal Scalded Skin Syndrome (SSSS)
Staphylococcal scalded skin syndrome (SSSS), also known as Ritter’s disease, was first described by German physician Gottfried Ritter von Rittershain in 1878. This condition primarily affects young children and is caused by toxins produced by Staphylococcus aureus. Outbreaks can occur in hospital nurseries.
Etiology
S. aureus produces exfoliative toxins that circulate in the bloodstream of affected individuals. There are two main types of these toxins: exfoliative toxin A (ETA) and exfoliative toxin B (ETB). These toxins cause a cleavage within desmoglein 1, a protein primarily located in the granular layer of the epidermis. This cleavage leads to the formation of superficial, fragile blisters that rupture easily, resulting in rapid desquamation (skin peeling).

Acne Vulgaris
Acne vulgaris is a common skin condition characterized by increased sebum production and inflammation of the pilosebaceous unit. It manifests with various lesions, including comedones, papules, pustules, nodules, and cysts, primarily localized to sebum-rich areas like the face, back, and chest.
Acne affects approximately 80% of adolescents, particularly during puberty. While not life-threatening, its persistent nature and the potential for scarring can significantly impact an individual’s quality of life and self-esteem.
Pathogenesis
Acne development is driven by three primary factors: increased sebum production, follicular hyperkeratinization, and the role of Propionibacterium acnes.
(a) Increased Sebum Production: Sebaceous glands are regulated by hormones, particularly androgens. These hormones stimulate sebaceous gland activity and hypertrophy, leading to a significant increase in sebum excretion.
(b) Follicular Hyperkeratinization: Hyperkeratinization of the follicular infundibulum leads to narrowing of the sebaceous duct. This obstruction prevents sebum from reaching the skin surface, resulting in its accumulation within the gland. Over time, this sebum becomes inspissated, forming comedones.
(c) Increased P. acnes Activity: P. acnes is a commensal bacterium that resides harmlessly on the skin. However, when follicular obstruction occurs, the resulting anaerobic environment, rich in sebum and cellular debris, promotes the proliferation and pathogenicity of P. acnes.
(d) Other Contributing Factors:
- Age: Acne is most prevalent in adolescents, with 90% of cases occurring between the ages of 13 and 19. While its severity typically diminishes with age, adult-onset acne can occur in individuals in their 20s, 30s, or even later.
- Gender: While acne is more common in females (female-to-male ratio of approximately 2:1), males tend to experience more severe forms.
- Family History: Genetics play a significant role in acne susceptibility. According to Goulden, 50% of acne patients have a positive family history.
- Climate and Ethnicity: Hot, humid, or dry climates can exacerbate acne. Caucasians and Asians are more prone to acne than individuals with darker skin tones.
- Occupation: Exposure to oil, grease, or excessive sunlight can increase the risk of acne.
- Stress: Stress can trigger or worsen acne breakouts.
- Diet: Certain foods, such as chocolate, sugar, butter, and coffee, may exacerbate acne in some individuals.
- Endocrine Disorders: Conditions like Cushing’s syndrome, hyperthyroidism, and polycystic ovary syndrome can contribute to acne development.
- Medications: Certain medications, including corticosteroids, isoniazid, halogens, androgens (testosterone), and lithium, can induce or worsen acne.
- Local Factors: Improper facial hygiene, excessive scrubbing, squeezing or picking at lesions, and overuse of cosmetics can negatively impact acne.
The antimicrobial efficacy of HOCl has been rigorously tested by the Cantacuzino Institute in Romania and the Functional Water Association of Japan, confirming its broad-spectrum activity and rapid bactericidal action. These studies highlight HOCl’s exceptionally high performance against Staphylococcus aureus and Pseudomonas aeruginosa, both frequent culprits in skin infections.
In a direct comparison with three commonly used skin antiseptics—5% povidone-iodine (Petadine, PI), 4% chlorhexidine gluconate (CHG, CHX), and 70% isopropyl alcohol (IPA)—HOCl at 100 ppm demonstrated immediate bactericidal activity against all tested organisms. This underscores its potential as a promising alternative skin cleanser, not only for its superior antimicrobial properties but also for its remarkable safety profile.
Our findings reveal that 100 ppm HOCl achieves an immediate kill time equal to or faster than 5% PI and 4% CHG against all tested microorganisms. While 70% IPA exhibits a faster immediate kill time compared to 4% CHG or 5% PI, its efficacy is comparable to 100 ppm HOCl for MSSA and shows limited activity against S. xylosus.
Importantly, HOCl demonstrates immediate killing activity against a range of bacterial strains implicated in skin infections, including drug-resistant varieties. (With the exception of methicillin-sensitive S. aureus, where HOCl’s kill time is comparable to other agents.)
Taken together, these results suggest that 100 ppm HOCl holds promise as a comparable, if not superior, alternative for skin antisepsis prior to procedures ranging from cosmetic injections to surgical interventions.

This data, from a 2018 study by Anagnostopoulos et al. titled “0.01% Hypochlorous Acid as an Alternative Skin Antiseptic: An In Vitro Comparison”, examines the in vitro effectiveness of common antiseptics against a range of skin-related microorganisms.
Microbial Targets:
- (A) Methicillin-resistant Staphylococcus aureus (MRSA)
- (B) Methicillin-sensitive Staphylococcus aureus (MSSA)
- (C) Methicillin-resistant Staphylococcus epidermidis (MRSE)
- (D) Methicillin-sensitive Staphylococcus epidermidis (MSSE)
- (E) Staphylococcus capitis
- (F) Staphylococcus xylosus
- (G) Candida albicans
- (H) Propionibacterium acnes, Corynebacterium striatum, Corynebacterium amycolatum, Streptococcus pyogenes, and Pseudomonas aeruginosa.
CFU: Colony forming units, a measure of viable bacterial or fungal cells.

MiraChlor Antiseptic Solution
Applications:
- Skin antisepsis: Effective for sanitizing various body areas.
- Surface disinfection: Suitable for use on all surfaces, including food contact surfaces, children’s toys, and personal belongings.
- Wound care: Helps prevent infection in minor cuts, scrapes, and burns.
- Odor elimination: Neutralizes odors in the air and on various surfaces, materials, and equipment.

MiraChlor antiseptic for medical use
. Disinfect before, during, and after surgery
. Disinfect wounds, ulcers, and surgical incisions